Social media can be an incredible resource for information related to skincare, as long as you’re consuming content from a trusted source (on that note, make sure you follow Renée Rouleau Skin Care on Tik Tok! I’ll be sharing some of my best skin tips, product recommendations, and more). However, as is typical of social media, trends come and go and certain products, ingredients, and skin concerns shift in and out of focus.
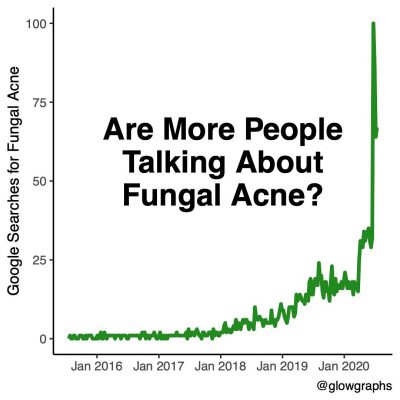
Take fungal acne for example. What was once a little-known skin condition has recently exploded in popularity (searches related to this topic are up 500%, according to Google Trends!). People are wondering what it is and whether it’s to blame for their bumps and breakouts. In this post, I’ll discuss the causes and characteristics of fungal acne as well as what to do if you think you have it. I’ll also share expert advice from Dr. Joshua Zeichner, an Associate Professor of Dermatology and the Director of Cosmetic & Clinical Research in Dermatology at Mount Sinai Hospital in New York City.
What Is Fungal Acne, and What Causes It?
Before we talk about what fungal acne is, we have to talk about what it isn’t. Believe it or not, fungal acne isn’t really acne at all—surprised?. That’s because acne is caused, in part, by P. acnes bacteria (read more about the science behind breakouts). This particular skin condition, on the other hand, is caused by an overgrowth of yeast, which is a fungus. Bacteria and fungi are two totally different things and they affect the skin in different ways.
“The term fungal acne is a misnomer because it’s not actually acne at all,” Dr. Zeichner explains. “Instead, this is a condition where yeast on the skin infects the hair follicles, leading to red bumps and pus pimples.” So, what’s referred to as fungal acne is actually a form of folliculitis (inflammation of hair follicles) caused by yeast. That explains why it’s commonly referred to as Pityrosporum folliculitis or Malassezia folliculitis. That also explains why it’s commonly found on areas like the chest, back, underarms, and scalp, since yeast require warm, moist environments to survive.
How Does Fungal Acne Differ from “Normal” Acne?
Aside from the fact that one is caused by a fungus, and the other is caused by bacteria, there are a few other distinctions between the two skin conditions. The first is that so-called “normal” acne is a chronic skin condition. Fungal acne, while often recurrent, isn’t chronic. The second is that fungal acne results in small, itchy, red bumps, unlike “normal” acne, which can result in papules, pustules, and nodules. (Learn how to clear the different types of clogged pores once and for all).
How Can I Tell If I’m Experiencing Fungal Acne?
Despite what social media might lead you to believe, fungal acne isn’t actually all that common. “While extremely popular on the internet, in reality, it is quite rare,” Dr. Zeichner says. “In the past decade, I can say that I’ve only seen it a handful of times. It is much more common in parts of the world where the weather is more humid, like in the Philippines.”
Since it’s relatively uncommon and it can be tricky to diagnose, it’s critical that you visit a dermatologist if you think you’re dealing with fungal acne. If your dermatologist finds that it’s indeed fungal acne, they will likely provide you with an antifungal medication. Using traditional acne products, which commonly contain antibacterial ingredients, won’t do much of anything. In some cases, it could actually make the situation worse by negatively affecting your microbiome and encouraging more yeast growth. So, if you have any suspicion at all that what you’re dealing with is fungal in nature, head to your dermatologist’s office. As Dr. Zeichner puts it, “knowing what you have means you can treat it the right way.”
Since the yeast that cause fungal acne are mostly lipid-dependent, meaning they require fatty molecules to survive, many people avoid using lipids in skincare. They avoid ingredients like linoleic and linolenic acids, oleic acid, castor oil, and polysorbates. They think doing this will prevent fungal acne by preventing the overgrowth of yeast in the first place. This simply isn’t accurate. The reality is that you need what I’ll call the perfect storm—just the right imbalance in your skin’s microbiome to allow for yeast overgrowth. Only then will you develop fungal acne. Plus, lipids can be really beneficial to the skin, helping to support your moisture barrier!
Why Is Fungal Acne Trending Right Now?
I believe this is such a hot topic right now because people who are prone to breakouts and blemishes aren’t happy with the results they’re getting from their current skincare routine, and they’re looking for a cure. The reality is that acne is a skin condition with no known cure, and just because your current routine isn’t working, doesn’t automatically mean you’re dealing with something that’s fungal vs. bacterial. Acne is stubborn, and it can be difficult to address, but it’s not impossible. Your best bet when dealing with acne is to use products that are formulated for your specific skin type. It’s also helpful to consult a skin expert, such as an esthetician or dermatologist, to develop a personalized approach.
There you have it. I hope this post has shed some light on fungal acne and why it’s trending on social media. I hope it also gave you insight as to why it’s probably not the missing piece to your acne puzzle.
Next, read all about skin acceptance and get tips from a therapist and top skin experts.
Celebrity Esthetician & Skincare Expert
As an esthetician trained in cosmetic chemistry, Renée Rouleau has spent 35 years researching skin, educating her audience, and building an award-winning line of products. Her hands-on experience as an esthetician and trusted skin care expert has created a real-world solution — products that are formulated for nine different types of skin so your face will get exactly what it needs to look and feel its best. Trusted by celebrities, editors, bloggers, and skincare obsessives around the globe, her vast real-world knowledge and constant research are why Marie Claire calls her “the most passionate skin practitioner we know.”



